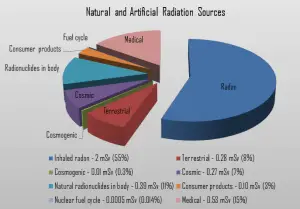
Radiation is used in a variety of medical examinations and treatments. Doses from medical radiation sources are determined by whether a person underwent a treatment or not. In general, radiation exposures from medical diagnostic examinations are low (especially in diagnostic uses). Doses may also be high (only for therapeutic uses). Still, in each case, they must always be justified by the benefits of accurate diagnosis of possible disease conditions or by benefits of accurate treatment. These doses include contributions from medical and dental diagnostic radiology (diagnostic X-rays), clinical nuclear medicine, and radiation therapy.
The medical use of ionizing radiation remains a rapidly changing field. In any case, the usefulness of ionizing radiation must be balanced with its hazards. Nowadays, a compromise has been found, and most of the uses of radiation are optimized. Today it is almost unbelievable that x-rays were, at one time, used to find the right pair of shoes (i.e., shoe-fitting fluoroscopy). Measurements made in recent years indicate that the doses to the feet were in the range of 0.07 – 0.14 Gy for a 20-second exposure. This practice was halted when the risks of ionizing radiation were better understood.
In the following points, we try to express enormous ranges of radiation exposure and a few doses from medical sources.
- 1 µSv – Eating one banana
- 1 µSv – Extremity (hand, foot, etc.) X-ray
- 5 µSv – Dental X-ray
- 10 µSv – Average daily dose received from natural background
- 40 µSv – A 5-hour airplane flight
- 100 µSv – Chest X-ray
- 600 µSv – mammogram
- 1 000 µSv – Dose limit for individual members of the public, total effective dose per annum
- 3 650 µSv – Average yearly dose received from natural background
- 5 800 µSv – Chest CT scan
- 10 000 µSv – Average yearly dose received from a natural background in Ramsar, Iran
- 20 000 µSv – single full-body CT scan
- 80 000 µSv – The annual local dose to localized spots at the bifurcations of segmental bronchi in the lungs caused by smoking cigarettes (1.5 packs/day).
- 175 000 µSv – Annual dose from natural radiation on a monazite beach near Guarapari, Brazil.
- 5 000 000 µSv – Dose that kills a human with a 50% risk within 30 days (LD50/30) if the dose is received over a very short duration.
As can be seen, low-level doses are common in everyday life.
Health Effects of Medical Exposures
The medical use of ionizing radiation remains a rapidly changing field. In each case, the usefulness of ionizing radiation must be balanced with its hazards. Nowadays, a compromise has been found, and most of the uses of radiation are optimized. We must emphasize eating bananas, working as an airline flight crew, or living in locations, and also increase your annual dose. Some medical treatments and diagnostic examinations also cause radiation doses. But it does not mean that it must be dangerous. In each case, the intensity of radiation also matters. It is very similar to heat from a fire (less energetic radiation). If you are too close, the intensity of heat radiation is high, and you can get burned. If you are at the right distance, you can withstand it without any problems, and it is comfortable. If you are too far from the heat source, the insufficiency of heat can also hurt you. In a certain sense, this analogy can be applied to radiation also from radiation sources.
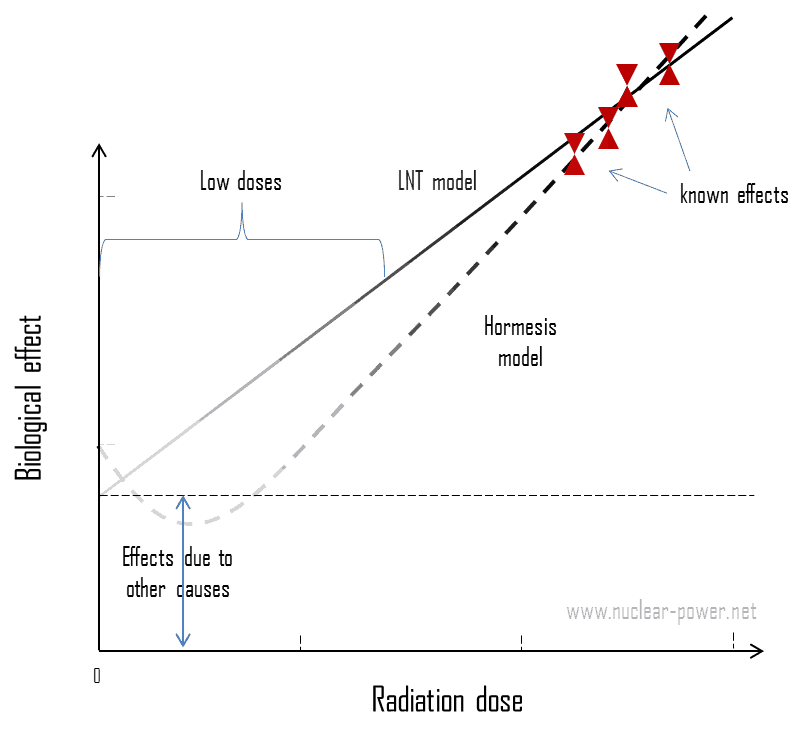
In some cases of medical exposures, we are talking (except radiotherapy) about so-called “low doses.” A low dose means additional small doses comparable to the normal background radiation (10 µSv = average daily dose received from natural background). The doses are very, very low, and therefore, the probability of cancer induction could be almost negligible. Secondly, and this is crucial, the truth about low-dose radiation health effects still needs to be found. It is unknown whether these low doses of radiation are detrimental or beneficial (and where is the threshold). Government and regulatory bodies assume an LNT model instead of a threshold or hormesis not because it is the more scientifically convincing but because it is, the more conservative estimate. The problem with this model is that it neglects many defense biological processes that may be crucial at low doses. The research during the last two decades is very interesting and shows that small doses of radiation given at a low dose rate stimulate the defense mechanisms. Therefore the LNT model is not universally accepted, with some proposing an adaptive dose-response relationship where low doses are protective, and high doses are detrimental. Many studies have contradicted the LNT model, and many have shown adaptive response to low dose radiation resulting in reduced mutations and cancers. This phenomenon is known as radiation hormesis.
Diagnostic X-rays – Radiation Doses
Diagnostic X-rays use a very small dose of ionizing radiation to produce pictures of the inside of the body. Diagnostic X-ray exams account for about 90% of the radiation dose the population receives from medical sources. Chest X-rays (about 100 µSv) are the most common, and they account for about 25% of all X-ray exams, followed by X-rays of the shoulder, pelvis, and limbs (another 25%) and dental X-rays (10%). Note that no direct evidence of radiation ever causing any harm at the exposure levels encountered with diagnostic radiological examinations.
X-rays belong to so-called low-LET radiation. Biological effects of any radiation increase with the linear energy transfer (LET) were discovered. In short, the biological damage from high-LET radiation (alpha particles, protons, or neutrons) is much greater than that from low-LET radiation (gamma rays, X-rays). This is because the living tissue can more easily repair damage from radiation spread over a large area than that concentrated in a small area. Of course, at very high levels of exposure, X-rays can still cause a great deal of damage to tissues.
Nuclear Medicine – Radiation Doses
Nuclear medicine is a medical science that involves the application of radioactive substances for diagnostic and treatment purposes. Nuclear medicine uses very small amounts of radioactive materials called radiotracers, which are taken internally, for example, intravenously or orally. Then, external detectors (gamma cameras) capture and form images from the radiation emitted by the radiotracers. Sometimes the radioactive drug can be used in the treatment itself: an example is the treatment of thyroid disease with I-131. Nuclear medicine imaging is unlike a diagnostic X-ray, where external radiation is passed through the body to form an image. It also provides unique information that often cannot be obtained using other imaging procedures.
The average effective dose for most nuclear medicine procedures varies between 0.3 and 20 mSv. The common bone scan with 600 MBq of technetium-99m has an effective dose of approximately 3.5 mSv. These doses can be compared with the average annual effective dose from the background radiation of about 3 mSv.
Radiation Therapy – Radiation Doses
In radiation therapy, the treatment aims to deliver a very high dose to the tumor but as little dose as possible to the surrounding healthy tissue. In this case, we are not talking about low doses. Using beams of high-energy gamma rays from cobalt-60 or accelerators, a localized high dose of radiation is delivered to the tumor, which tends to kill tumor cells. The amount of radiation used in photon radiation therapy is measured in grays (Gy) and varies depending on the type and stage of the cancer being treated.
For curative cases, the typical dose for a solid epithelial tumor ranges from 60 to 80 Gy (locally), while lymphomas are treated with 20 to 40 Gy. Note that this is not the effective dose. A gray is a unit of absorbed dose, defined as the amount of energy deposited by ionizing radiation in a tumor.